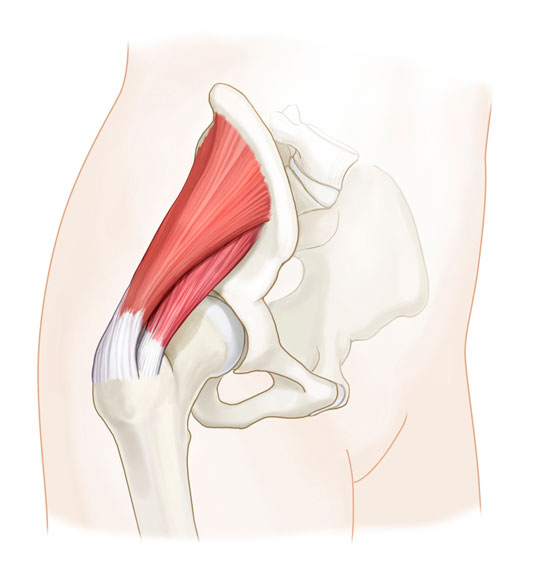
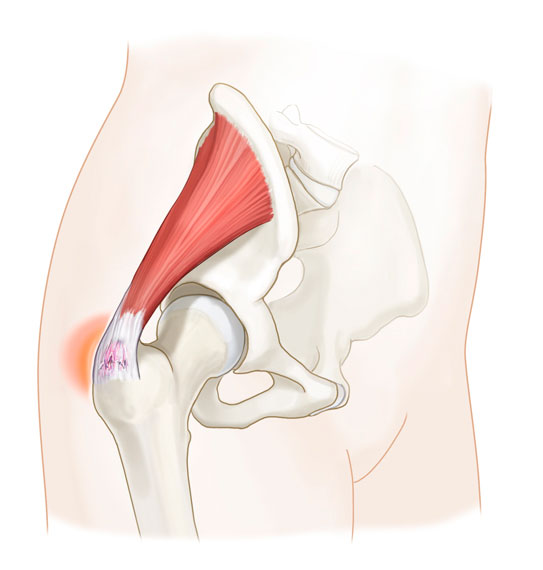
Abductor tendon problems are a common source of Greater Trochanteric Pain Syndrome (GTPS) that fails to respond to conservative treatment, often described erroneously as “recalcitrant trochanteric bursitis”. The gluteus medius is the more frequently involved of the two. These tendon problems range from tendinitis to partial or complete tendon tearing. Tears can occur from an acute injury, but often occur as an attritional process with age, especially over the age of 40. In fact, attritional tearing is sometimes seen coincidentally on imaging studies, such as MRI, where it is not even causing symptoms.
Tendinitis mostly responds to usual conservative measures, including activity modification, supervised physical therapy, nonsteroidal anti-inflammatory medication and, lastly, judicious use of a cortisone injection. Painful tendon tears may also respond to nonsurgical treatment, and there are other types of injectable products that can be tried, including platelet rich plasma (PRP) and stem cells. Sometimes, tendon healing can be jumpstarted with resolution of symptoms. For those that fail efforts at nonsurgical treatment, surgery to repair or reconstruct the tendon damage may be an option, with various endoscopic and open treatments available, depending on the magnitude of the damage.
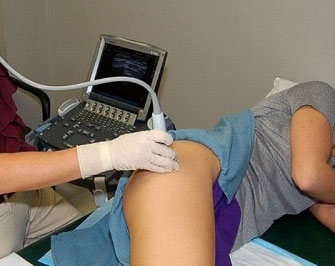
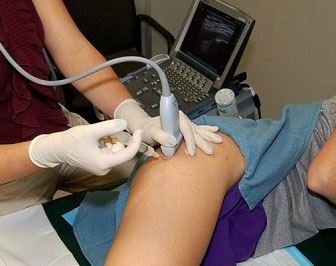
Diagnosing problematic abductor tears can be tricky. Tendon problems are often seen on MRI and by ultrasonic inspection. In fact, ultrasound guided injections are a mainstay in confirming the diagnosis as well as a last line of conservative treatment. (Related Study: Perioperative Care) Assessing these problems requires a clinician knowledgeable and experienced in these and other hip disorders. The symptoms can overlap with other problems, and other joint problems may coexist with painful tendon lesions. Treatment often involves sorting out the various contributing components and prioritizing which needs the most specific attention.
Video deomnstrtes injection of a gluteal tear, which literally takes seconds.
Location
2004 Hayes Street
Suite 700
Nashville, TN 37203
Office Hours
Monday-Friday:
8:00 am – 5:00 pm